3 results
Characteristics of patients admitted to a Psychiatric Home Hospitalization Unit and burden felt by caregivers
- J. Marti-Bonany, O. Garcia, D. Tolosa, R. Romar, G. Mateu, D. Garcia, R. Sanchez, M. G. Hurtado, M. Campillo, C. Monserrat, M. Roldan
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S901
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Severe mental illnesses characterized by periods of relapse that require intensive resource management. Caregivers of schizophrenia and bipolar disorder patients feel a considerable burden of care (Tanna et al. Ind Psychiatry J 2021, 30(2):299-304).
The main objective of Hospital at home for psychiatric patients is to provide intense care to patients with severe mental disorders at home as an alternative to acute admission (Alba et al. Rev Psiquiatr Salud Ment. 2019, 12 (4) 207-212).
ObjectivesThe aim of this study is to describe the characteristics of patients attended at the Psychiatric Home Hospitalization Unit of our hospital (HAD-CAEM) and to assess the of burden of care that caregivers feel while giveing care to this patients.
MethodsData were collected retrospectively at admission and discharge of all patients treated at HAD-CAEM between August 2018 to March 2022. Incomes of patients who met DSM-5 criteria for schizophrenia, bipolar disorder and major depressive disorder. Severity of disease and patient’s level of functionality was evaluated with the global assessment of functioning scale (GAF) and the Clinical Global Impression Scale (CGI). Burden Caregivers was evaluated with The Zarit Caregiver Burden Scale (ZCBS). Statistical analysis was performed by using SPSS program.
Results109 patients were included in the study. 49.5% were women. The mean age was 48 years (SD 18.47 years). 44% met criteria for schizophrenia, 25.7% for depressive disorder, and 30.3% for bipolar disorder. Most of them lived with their own family (47.7%); had secondary education (51.4%) and were unemployed (33%). 81% had a history of at least one admission to an acute psychiatric unit.
The mean duration of admission in HAD-CAEM was 33.8 days (SD 15.72 days), with a mean follow-up of 8.75 visits (SD 3.58 visits).
The mean CGI severity item at admission was 4.36 and there was an improvement at the time of discharge according to the CGI improvement item (mean CGI-I=2.43).
The GAF scale on admission was 46.74 (SD 11.2) and on discharge 64.24 (SD 13.85), showing an improvement of 17.5 points at discharge (p<0.001).
The mean ZCBS of the sample was 48.21 (SD 15.11). Mean ZCBS in Schizophrenia group (n=22) was 46.13 (SD 16.53), in depressive group (n=18) was 43.61 (SD 12.89) and for bipolar group (n=17) was 55.76 (SD 13.19). A statistical test is performed with ANOVA, showing significant differences between groups (p=0.039). Post-hoc analyzes show significant differences between bipolar disorder group and the depressive disorder group (p=0.04). No significant differences are found between the other groups.
ConclusionsCaregivers of schizophrenia, depressive and bipolar disorder patients feel a considerable burden of care. ZCBS was administered to the caregivers on the last day of admission, when the patient presented clinical and functional improvement. More studies are needed to support these results.
Disclosure of InterestNone Declared
Patient satisfaction in an “open-door” acute inpatient psychiatric unit
- M. Campillo, L. Rius, S. Garcia, M. Olivero, G. Sanchez Tomico, M. Martinez Garcia, I. Garcia Velasco, C. Monserrat, A. Pratdesava, R. Sanchez
-
- Journal:
- European Psychiatry / Volume 66 / Issue S1 / March 2023
- Published online by Cambridge University Press:
- 19 July 2023, p. S903
-
- Article
-
- You have access Access
- Open access
- Export citation
-
Introduction
Traditionally, psychiatric wards had established a “locked door” policy but secluded conditions may increase patient’s discomfort1 that could affect the perception of health quality of care2. Recently, the “open-door” policy is being adopted in several European countries but its impact on patient satisfaction remains unknown (Schreiber, LK. BMC Psychiatry. 2019 May 14;19(1):149). Since 2019 our psychiatric hospital has implemented the open-door policy.
ObjectivesThe aim of this study is to investigate the impact of the “open-door” policy on patient satisfaction during their stay in the acute inpatient unit of our psychiatric hospital.
MethodsThis is an observational study. Prior to the implementation of the open door policy 31 patient satisfaction data was collected between October 2018 to April 2019 and it was also assessed with 31 subjects between July to October 2019, after the implementation of the open “door-policy”. The inclusion criteria were being >18 years old, reading Spanish correctly and with a length of stay >72 hours. The patients with dementia disorder and intellectual disability where excluded from the study. We used the Satispsy-22-E scale, a self-administered questionnaire (Frías, V., et al. 2018. Psychiatry Res. Oct;268:8-14). It assesses patient’s experience of hospitalization through 22 items distributed into 6 dimensions. The score range is from 0 to 100. Differences in Satispsy-22-E scores were analysed by applying ANOVA using the IBM-SPSS (v. 25).
ResultsTotal scores in Satispsy-22 are provided in Figure 1. We found that patient satisfaction was increased in the dimensions of “personal experience” and “food” (p<0.05). No significant differences were found in staff, quality of care, information, activity dimensions and Total score (Table 2).
Dimension F-Test Statistic Value Staff 1.402 p=0.241 Quality of Care 841 p=0.362 Personal Experience 4.071 p=0.048* Information 656 p=0.420 Activity 434 p=0.512 Food 4.507 p=0.037* TOTAL 3.645 p=0.61 Image:
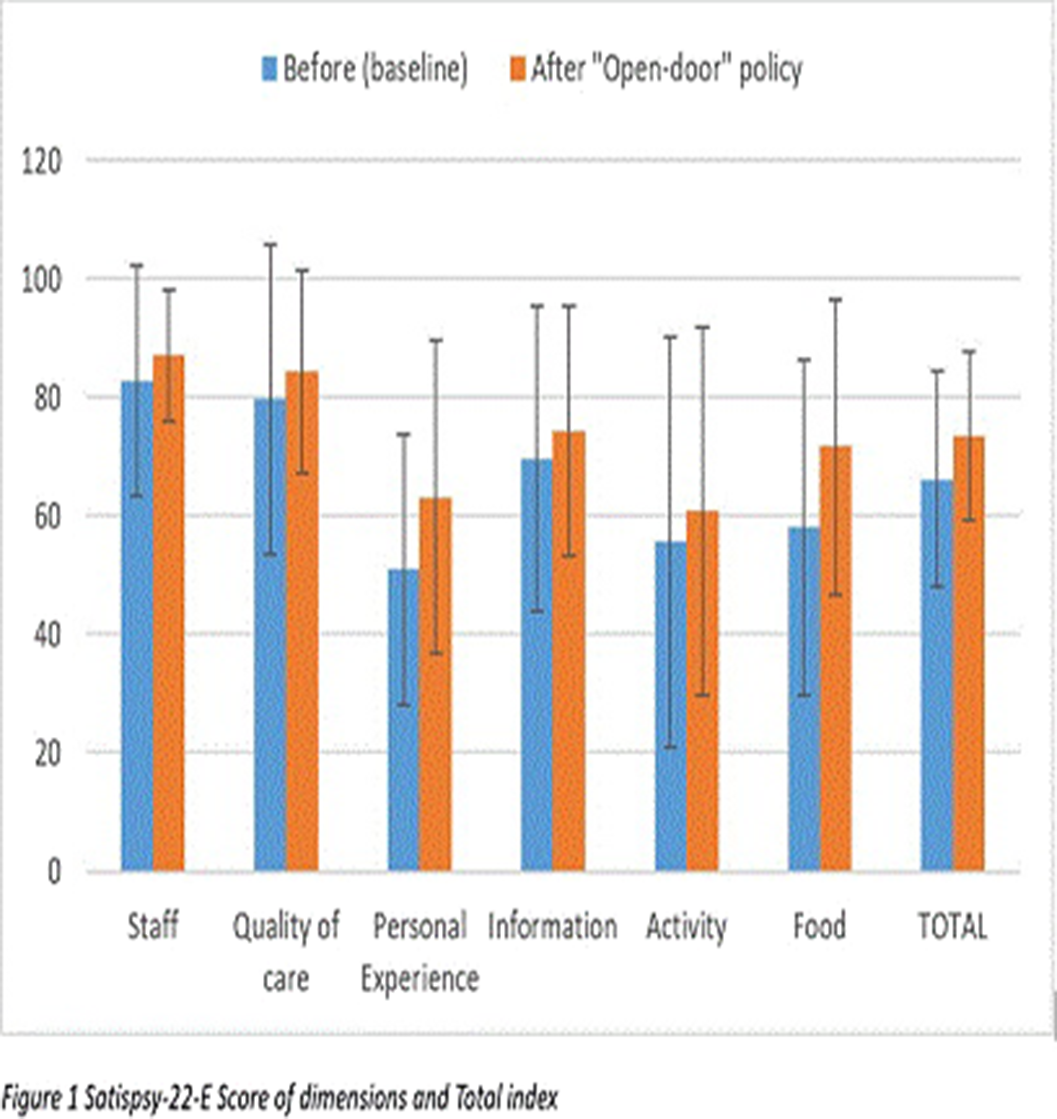 Conclusions
ConclusionsOur results provide preliminary evidence indicating that the open-door policy could have a positive impact on patient satisfaction, especially in relation to the personal experience on an acute inpatient psychiatric unit.
Disclosure of InterestNone Declared
Synthesis of Hard Nitride Coatings by ion Beam Assisted Deposition
- J. D. Demaree, C. G. Fountzoulas, J. K. Hirvonen, M. E. Monserrat, G. P. Halada, C. R. Clayton
-
- Journal:
- MRS Online Proceedings Library Archive / Volume 504 / 1997
- Published online by Cambridge University Press:
- 10 February 2011, 271
- Print publication:
- 1997
-
- Article
- Export citation
-
Ion beam assisted deposition (IBAD) has been used to deposit chromium nitride coatings using 1200 eV nitrogen ions from an RF-type ion source and thermally evaporated chromium. The ion/atom arrival ratio R was varied from 0 to 8 to modify the coating composition, microstructure, growth rate and stress state in order to optimize the properties of the material for use as a possible substitute for electroplated chromium in a number of anti-corrosion and tribological applications. The coatings were examined using Rutherford backscattering spectrometry and x-ray photoelectron spectroscopy, and contained up to 44 at % nitrogen in a mixture of bcc Cr-N, Cr2N, and CrN. The microstructure of the coatings was examined by scanning electron microscopy, and the tribological behavior of the coatings was examined using an automated scratch testing and nanoindentation. XPS examination of the coatings indicates that nitrogen near the surface was bound to the metal as CrN and Cr2N in most of the coatings studied by XPS, which is expected to significantly affect their corrosion behavior. The high R values needed to form large amounts of the CrN phase in the bulk of the coating causes significant sputtering during deposition. This study indicates that it is not possible to form a coating consisting solely of cubic CrN by IBAD under these experimental conditions (room temperature substrate and partial pressure of nitrogen of 1.8 × 10−2 Pa). Nevertheless, the IBAD coatings produced were hard, in a compressive stress state, and highly adherent, all properties that make them candidates for use in selected Army applications.




